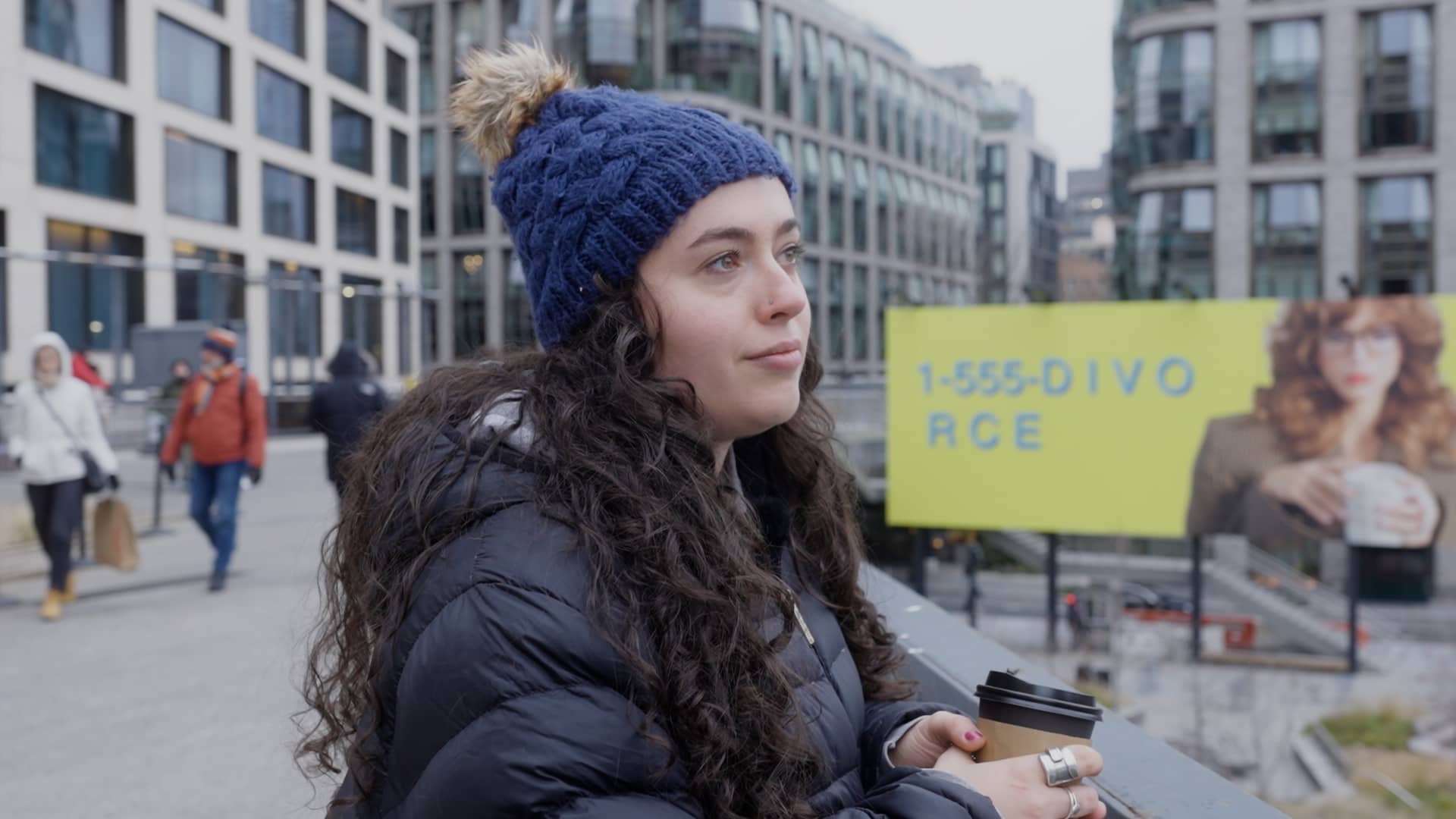When Eileen Tyrrell logged into New York state’s health insurance marketplace in December, she says her monthly premium jumped from about $147 to $849.
“It was one of those moments where your stomach drops,” says Tyrrell, 26, who earned about $53,000 in 2025 as a bookstore manager in Brooklyn. She expects to earn around $72,000 in 2026, including her bookstore salary and income from content creation on TikTok.
Last year, federal premium tax credits covered about $510 of Tyrrell’s monthly premium, bringing the out-of-pocket cost of her Affordable Care Act bronze plan down to $147 a month. But between her higher income leading to a larger base premium and the expiration of enhanced pandemic-era subsidies, the same plan would cost her hundreds more per month.
The enhanced subsidies, first expanded in 2021 under the American Rescue Plan Act, removed the income cutoff for financial assistance and capped premiums at 8.5% of a household’s income, allowing more middle-income Americans to qualify for help.
However, Congress did not extend the provisions beyond 2025. While premium tax credits can still lower monthly costs for some Americans, eligibility is limited to households earning up to 400% of the federal poverty level — $62,600 for a single person in 2025 — a cutoff that was temporarily eliminated under the enhanced subsidies.